Acne is a skin disease caused by inflamed pilosebaceous follicles (the glands secreting sebum at the root of the hair) with the formation of comedones.
Etymology
The word acne is a form of the Greek word akme, which means summit peak.
Epidemiology
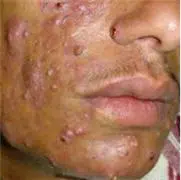
Acne is an unfortunate rite of passage in the adolescence of 85% of people of all ethnic groups. Acne primarily affects teenagers and usually stops spontaneously at the end of adolescence.
Causes
Genetic factors are the only confirmed cause to date, but stress, hygiene, environment and diet may also indirectly affect the appearance of acne.
Pathophysiology
Hyperseborrhea
Hyperseborrhea is the excessive production of sebum which gives the characteristic shiny appearance to the skin of acne sufferers. Sebum serves to protect the skin from external erosion, forming a thin lipid film on its surface. During puberty, the sudden increase in the rate of circulating hormones (testosterone in particular) causes an excess of activity of pilosebaceous glands (via the enzyme 5-alpha reductase).
The obstruction of the follicles
Excess cell formation promotes the overproduction of sebum and hence the proliferation of white dots on the skin surface. The thickening of the outer portion of the gland can also cause inflammation of the hair follicles. The obstruction of a gland filled with an excess of sebum leads to the appearance of a comedo, which becomes a blackhead when the keratin from the dead cells contained in it is oxidized.
The proliferation of bacteria
Propionibacterium acnes is a bacteria that lives normally in everyone, in the hair follicles. It does not cause infection, but exacerbates inflammation of follicles that have an excess of sebum, causing the characteristic red bumps.
Other factors
- Familial traits (genes) have been suggested as a causal factor.
- Hormonal factors are also important: acne is most common in young men, with relative exacerbation in women during menstruation . Acne typically appears during puberty, when hormonal upheaval is at its greatest.
- Stress is suspected, but there have been no detailed studies to confirm whether it is a serious contributory factor.
- Exposure to the sun : the sun thickens skin and aggravates acne, despite a transient improvement at the beginning of exposure (due to the bactericidal effect of UV radiation and the color of tanned skin that reduces the appearance of lesions).
- Exposure to certain pollutants, including chlorine. Some pesticides, perhaps because of their action as endocrine disruptors, seem able to trigger episodes of a form of acne called chloracne – the Seveso disaster triggered an outbreak of chloracne in the population when dioxins leaked into the environment.
- Eating chocolate, cold cuts or high-fat foods do not cause acne, although this myth is very persistent. However, recent studies have shown a link between acne and the consumption of foods of high glycemic index and high consumption of milk (especially skim milk and semi-skimmed). These foodstuffs are believed to act through the hormone IGF-1 which stimulates the synthesis of androgens and hence cell proliferation in the sebaceous glands.
Typical Forms
The regions of the body most frequently affected are the face, neck, chest , shoulders, and back.
- Seborrhoea (oily skin)
- Comedones and blackheads
- Papules: These are bumps in the skin that are inflamed (red, hot, swollen, sometimes painful), which follow a comedo (microcyst) less than 5mm in diameter. They disappear on their own, or give a pustule.
- Pustules: they contain a yellow purulent content.
- Nodules: the nodules are inflammatory lesions wider than 5 mm in diameter. They eventually rupture and leave a scar on the skin.
Special Forms
Nodular Cystic Acne
Combines all lesions, with large numbers of pustules and scars, reaching the trunk, back, buttocks and sometimes the top of the labia majora in women.
Acne Conglobata
Very severe acne, accompanied by diaphoresis, and of prolonged duration. We distinguish between elementary lesions, associated with abscesses , and fistulas , with scars digging into the skin or in relief (Keloid Scars). It causes major social disability and must be treated quickly and effectively.
Other forms
- Neonatal acne
- Acne caused by drugs (estrogen-progestin, corticosteroids , anti-epileptic drugs, androgens , lithium , …)
- Occupational acne (oils, cosmetics, …)
- Acne secondary to systemic disease ( hormonal disease , Stein-Leventhal syndrome , hirsutism , …)
- Acne caused by rosacea (rosacea)
Treatment

If drug treatment is being considered it should only be done in consultation with a physician. Treatment is also based on good hygiene (cleaning of the skin) and in all cases must be continued for a prolonged period (several months or even years) to be fully effective.
There are products that address the bacteria often associated with acne (Propionibacterium acnes), while others act on the mediators of inflammation, such as nicotinamide, a molecule that occurs naturally in many foods. Zinc can reduce the secretion of sebum.
Oily skin, blackheads, cysts
- Treatment with retinoids.
Example: Vitamin A acid cream once a day in the evening on clean dry skin. Side effects: irritation at the beginning of treatment, eczema (rare), photosensitivity (sun intolerance) and teratogenicity (malformation of a foetus before birth) – do not take during pregnancy and seek advice from a pharmacist .
Papulopustular acne
Benzoyl peroxide + a general antibiotic (to fight against Propionibacterium acnes) such as the cyclins (tetracyclines). Propionibacterium acnes is however becoming increasingly resistant to the tetracyclines.
- Contra indications for cyclin treatment: pregnancy, association with isotretinoin, children under 8 years.
- Possible side effects: photosensitivity, gastrointestinal disturbances.
Severe acne or acne resistant to long term antibiotic therapy
Isotretinoin is a form of vitamin A, an anti-inflammatory and very powerful inhibitor of sebum secretion. As already mentioned, this product is teratogenic (risk of fetal malformations). In women, treatment must always be associated with contraception (at least 1 month before and 1 month after treatment) and it is recommended to do a pregnancy test before starting treatment and then once a month.
- Side effects: risk of fetal malformation, dry skin and mucous membranes, joint pain, liver problems, temporary worsening of acne in the early treatment
Acne in women (not pregnant)
Acetate cyproterone + ethinyl estradiol (which corresponds to the prescription of a contraceptive pill ) in addition to creams.
Infant Acne
Infant acne is general of short duration (4-12 weeks) so the best course of action is to leave it to subside naturally.
Other treatments
Zinc has shown some efficacy in inflammatory acne.
To reduce existing scars: healing creams at first, then the use of peeling effect creams. The visual appearance of scars is generally reduced over time.